The big picture
What services does Openground offer?
Openground is an Australia-wide charity for human flourishing. We embrace a holistic and user-friendly approach to health - mental, emotional, physical and spiritual. We offer big discounts for those in need. We provide evidence-based programs drawing on intensive mindfulness meditation training as well as active exploration of patterns of thinking, feeling, sensing to empower people to take wise action. Our programs offer a step-by-step training to support clarity, emotional regulation and mental clarity. People learn specific skills and practices to help break cycles of anxiety, distress, unhappiness and exhaustion.
Who for?
Our programs are trans-diagnostic and can effectively help with all kinds of human stress: burnout, traumatic stress, anxiety, depression, emotion dysregulation, negative thoughts, experiential avoidance and interpersonal problems. They can also be very helpful for people with behavioral problems and recovery from substance abuse, as well as dealing with physical illness that generate mental and emotional suffering. An 8 week mindfulness training can also assist people in being able to more effectively use therapy as it increases awareness of emotions and thoughts and undermines reactivity. See below for a summary of evidence for Mindfulness Based Programs.


Empowering collaboration
To help people build healthy, strong wise minds we endeavour to:
- Offer skills, knowledge and a collaborative process to draw out people’s own innate wisdom in meeting their own challenges
- Embody trauma-sensitive care every step of the way
- Complement conventional healthcare and support the effectiveness of other therapy or medication they are using and collaborate with other healthcare providers.
- Provide an environment of safety and trust where connection can happen and where a sense of isolation can soften.
- Acknowledge and work with the societal causes of mental and physical suffering.
- Enhance positive capacities such as self-compassion, well-being, and self-worth.
- Provide an ongoing sense of community through ongoing practice and follow on courses
Do be in touch if you wish to speak to an experienced teacher about someone you wish to refer.
2009 study of 28 Openground MBSR courses exploring the mechanisms of mindfulness
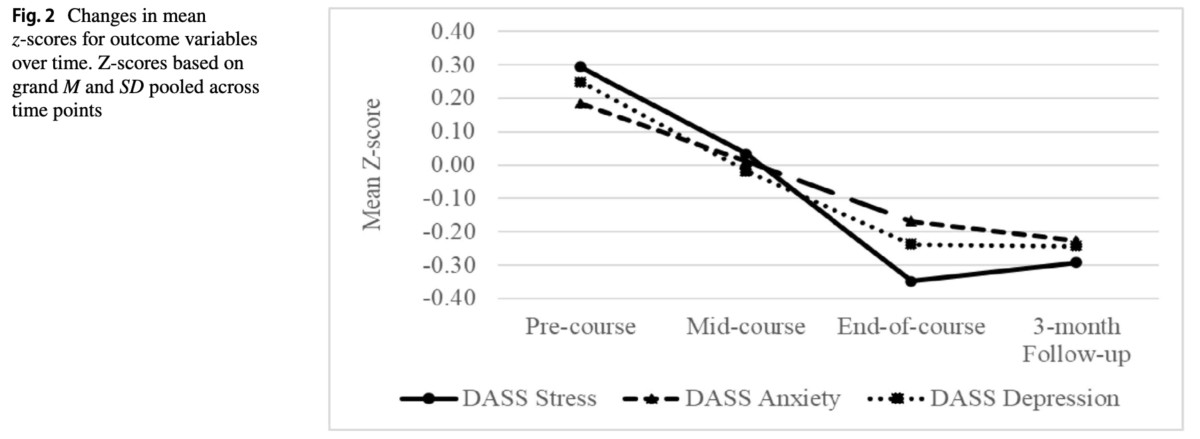
Mindfulness Based Programs: theory, practice and pedagogy
MBPs:
- Are informed by theories and practices that draw from a confluence of contemplative traditions, science, and the major disciplines of medicine, psychology and education.
- Are underpinned by a model of human experience which addresses the causes of human distress and the pathways to relieving it.
- Develop a new relationship with experience characterized by present moment focus, de-centring, and an "approach" orientation.
- Support the development of greater attentional, emotional and behavioral self-regulation, as well as positive qualities such as compassion, wisdom, equanimity.
- Engage the participant -
-
- in a sustained intensive training in mindfulness meditation practice
- in an experiential inquiry-based learning process, an
- in exercises to develop insight and understanding. (Crane et al, 2017)
-
What is the evidence that Mindfulness Based Interventions help people?
-
Overview of the evidence for Mindfulness Based Interventions
Research studies around the world have shown that mindfulness can assist people to feel less stressed, less anxious or depressed, and more able to engage with life, no matter how difficult or challenging things may be.
There are thousands of peer-reviewed scientific papers reporting the effects of various approaches to mindfulness courses or programs for physical, mental, cognitive and social health. An article published in 2017 by Professor David J Creswell, of Carnegie Melon University provides an excellent starting point. In Mindfulness Interventions (1), Creswell assesses the strength and quality of evidence for MBIs in each of these health domains. We have drawn on Creswell’s article and augmented this work with more recent evidence.
At this point in time the strongest evidence is in support of the standardised 8-week MBI training protocols (Mindfulness Based Stress Reduction and Mindfulness Based Cognitive Therapy) for improving mental health, followed by physical health, then social, cultural and cognitive outcomes.
We refer throughout to mindfulness-based interventions (MBIs). These are courses or programs of activity that teach the skills and practices of mindfulness. The evidence reported below is (except where stated) based on randomised controlled trials (RCTs). This is a type of study that collects data for pre-defined outcomes (like stress, mindfulness, markers of physical health, cognitive function, etc) from a study sample before and after an MBI.
Importantly, the RCT sample involves at least two groups of people with similar characteristics and contexts; one does the MBI, the other group acts as the control group. Control groups for MBI research can be active (e.g. other psychological treatments, physical exercise, etc) or inactive (e.g. treatment as usual). RCTs give the best evidence of causality, because if all other factors are held constant, the differences between the two groups at the end of the training can be attributed to the MBI. Meta analyses and systematic reviews pool together the findings from multiple RCTs to show the overall quality of evidence and effectiveness of MBIs across different outcomes, settings, samples and contexts.
Current studies are addressing evidence gaps, including the potential of mindfulness and MBIs
in public health, dementia prevention, political, environmental and social policy, and in supporting psychosocial safety in workplaces, schools and other social settings.
This summary has been collated by Dr Larissa Bartlett PhD 24 April 2024. -
Mindfulness for mental health?
RCT evidence shows MBI participants experience reduced depression relapse rates and substance use, and improved adherence to treatment for drug addiction (3). Reductions in anxiety, depression, and PTSD symptomatology are commonly reported following MBI participation (4). In some clinical contexts, MBIs can offer similar or additional long-term benefits compared to gold-standard treatments (e.g., antidepressants, relapse prevention programs, CBT). When offered as a non-clinical intervention in workplace settings, MBIs consistently improve stress and related mental health problems (5).
-
Mindfulness interventions for cognition and mood?
MBIs can improve attention-related outcomes (e.g., sustained attention, working memory) and affective outcomes (e.g., reducing rumination) in students and the skills and practices of mindfulness are commonly applied in school systems. MBIs also consistently appear to cultivate positive psychological capital (a composite of hope, self-efficacy, resilience and optimism) (6), which is associated with positive leadership, problem solving and performance in workplace contexts. Trait mindfulness has been shown to be associated with less cognitive decline and less Aβ and tau (amyloid-β (Aβ) peptides for plaques and tau for tangles) in the brain in older adults at risk for Alzheimer’s Disease (7) however evidence of changes in these markers in response to MBIs is limited (8).
-
Mindfulness for physical health?
Mindfulness Based Intervention (MBI) participants experience improved chronic pain management relative to usual treatment. Results from MBI RCTs showed effects superior to some active treatments (support groups, health education programs) and equivalent to others (e.g. cognitive behaviour therapy, CBT). Since 2021, MBIs have been an evidence-based first-line intervention tool for improving physical and psychological wellbeing in cardio-vascular disease patients (2). There is also promising evidence that mindfulness interventions may improve immunity, reduce symptoms and improve quality of life across a broad range of stress-related conditions (e.g., fibromyalgia, IBS, breast cancer, psoriasis). At the time of publishing this article, relatively little is known about how MBIs affect health behaviours.
-
Mindfulness interventions for social and cultural transformation?
There is an emerging body of research on interpersonal and prosocial effects of MBIs, with studies pointing to improved relational outcomes (e.g., relationship satisfaction and prosocial behaviours). This has been shown in patient- clinician, student-teacher, parent-child and intimate partner settings (9). Emerging evidence supports mindfulness interventions for cultivating adaptive leadership and workplace psychosocial safety (10); and higher mindfulness as a sociocultural typology is associated with progress toward sustainable development goals at national levels (11).
-
References
1: Creswell JD. Mindfulness Interventions. Annu Rev Psychol. 2017 Jan 3;68:491-516. doi: 10.1146/annurev-psych-042716-051139. Epub 2016 Sep 28. PMID: 27687118.
2: Marino F, Failla C, Carrozza C, Ciminata M, Chilà P, Minutoli R, Genovese S, Puglisi A, Arnao AA, Tartarisco G, Corpina F, Gangemi S, Ruta L, Cerasa A, Vagni D, Pioggia G. Mindfulness-Based Interventions for Physical and Psychological Wellbeing in Cardiovascular Diseases: A Systematic Review and Meta-Analysis. Brain Sci. 2021 May 29;11(6):727. doi: 10.3390/brainsci11060727. PMID: 34072605; PMCID: PMC8227381.
3: Kuyken W, Byford S, Taylor RS, Watkins E, Holden E, White K, Barrett B, Byng R, Evans A, Mullan E, Teasdale JD. Mindfulness-based cognitive therapy to prevent relapse in recurrent depression. J Consult Clin Psychol. 2008 Dec;76(6):966-78. doi: 10.1037/a0013786. PMID: 19045965.
4: Janssen M, Heerkens Y, Kuijer W, van der Heijden B, Engels J. Effects
of Mindfulness-Based Stress Reduction on employees’ mental health: A systematic review. PLoS One. 2018 Jan 24;13(1):e0191332. doi: 10.1371/journal. pone.0191332. PMID: 29364935; PMCID: PMC5783379.
5: Bartlett L, Martin A, Neil AL, Memish K, Otahal P, Kilpatrick M, Sanderson
K. A systematic review and meta-analysis of workplace mindfulness training randomized controlled trials. J Occup Health Psychol. 2019 Feb;24(1):108-126. doi: 10.1037/ocp0000146. PMID: 30714811.
6: Roche M, Haar JM, Luthans F. The role of mindfulness and psychological capital on the well-being of leaders. J Occup Health Psychol. 2014 Oct;19(4):476-89. doi: 10.1037/a0037183. Epub 2014 Jun 16. PMID: 24933594.
7: Strikwerda-Brown C, Ozlen H, Pichet Binette A, Chapleau M, Marchant NL, Breitner JCS, Villeneuve S. Trait Mindfulness Is Associated With Less Amyloid, Tau, and Cognitive Decline in Individuals at Risk for Alzheimer’s Disease.
Biol Psychiatry Glob Open Sci. 2022 Jan 17;3(1):130-138. doi: 10.1016/j. bpsgos.2022.01.001. PMID: 36712573; PMCID: PMC9874144.
8: Schlosser M, Demnitz-King H, Barnhofer T, Collette F, Gonneaud J, Chételat G, Jessen F, Kliegel M, Klimecki OM, Lutz A, Marchant NL; Medit-Ageing Research Group. Effects of a mindfulness-based intervention and a health self-management programme on psychological well-being in older adults with subjective cognitive decline: Secondary analyses from the SCD-Well randomised clinical trial. PLoS One. 2023 Dec 15;18(12):e0295175. doi: 10.1371/journal. pone.0295175. PMID: 38100477; PMCID: PMC10723715.
9: Singh NN, Lancioni GE, Winton AS, Curtis WJ, Wahler RG, Sabaawi M, Singh J, McAleavey K. Mindful staff increase learning and reduce aggression in adults with developmental disabilities. Res Dev Disabil. 2006 Sep-Oct;27(5):545-58. doi: 10.1016/j.ridd.2005.07.002. Epub 2005 Sep 26. PMID: 16188424.
10: Roussel L. Leadership’s Impact on Quality, Outcomes, and Costs. Crit Care Nurs Clin North Am. 2019 Jun;31(2):153-163. doi: 10.1016/j.cnc.2019.02.003. Epub 2019 Apr 8. PMID: 31047090.
11: GBD 2019 Under-5 Mortality Collaborators. Global, regional, and national progress towards Sustainable Development Goal 3.2 for neonatal and child health: all-cause and cause-specific mortality findings from the Global Burden of Disease Study 2019. Lancet. 2021 Sep 4;398(10303):870-905. doi: 10.1016/ S0140-6736(21)01207-1. Epub 2021 Aug 17. PMID: 34416195; PMCID: PMC8429803.


